Idiopathic Pulmonary Fibrosis (IPF) Overview
This information was reviewed and approved by Jeffrey James Swigris, DO, MS (9/1/2017).
- Do not delete this
What is Idiopathic Pulmonary Fibrosis or IPF?
Idiopathic pulmonary fibrosis (IPF) is the most common type of interstitial lung disease [AT1] (ILD). “Idiopathic” means the cause is unknown. Pulmonary refers to the lungs, and “fibrosis” is scarring.
Idiopathic pulmonary fibrosis, or IPF, is a scarring disease of the lung. So this is a disease in which the normal sponge or meaty part of the lung becomes scarred or fibrotic.
The cause is unknown, thus the name is idiopathic. There are a number of different causes for pulmonary fibrosis, but idiopathic pulmonary fibrosis is a specific diagnosis that has a specific pattern, either on CT scan or surgical lung biopsy.
In idiopathic pulmonary fibrosis, as in other forms of ILD, there is an abnormality in the interstitium of the lung. The interstitium refers to the microscopic area within the walls of the alveoli (air sacs). Like leaves on a tree arise from the smallest twigs, the alveoli arise from the tiniest airways in our lungs (bronchioles).
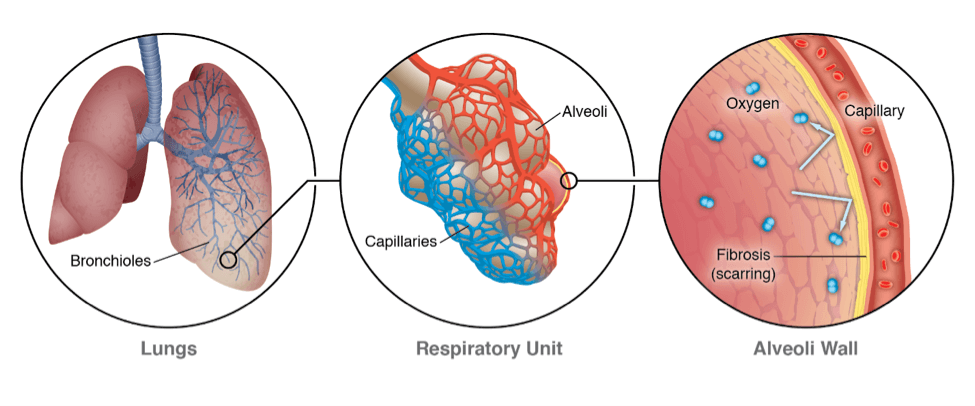
Each lung has about 400 million alveoli. Each one is incased in a meshwork of tiny blood vessels (capillaries). Together, an air sac and its blood vessels make up a respiratory unit, which is where oxygen is getting into the bloodstream and carbon dioxide is leaving the bloodstream.
To get into the bloodstream, the oxygen must make its way from inside the air sacs into the tiny blood vessels that surround the air sac. Oxygen does this by traveling through the wall of the air sac, through the super thin layer between the air sac and the surrounding blood vessels, and then through the wall of the blood vessel. That thin layer between the wall of the air sac and the blood vessels is the interstitium.
In all ILDs, including IPF, the normally thin interstitium is thickened by inflammation or fibrosis (or both). Thickening of the interstitium by inflammation or fibrosis causes two problems:
- The air sacs become stiff and can’t expand, so they can’t hold as much air as a normal air sac; and
- Oxygen can’t cross the thickened interstitium to get into the blood vessel.
So, lungs with IPF are stiff. They don’t hold as much air as a normal lung, and they don’t allow oxygen into the bloodstream like a normal lung.
There is still a lot to learn about IPF. We do know that IPF usually gets worse over time, and people with IPF usually do not live as long as people who don’t have IPF. But, accurately predicting how long a patient with IPF will live is impossible.
Signs and Symptoms
The first symptom that usually occurs with IPF is shortness of breath with activity. Other common symptoms of IPF are a dry, hacking cough and fatigue.
Most often, the symptoms of IPF come on and get worse gradually over months or a few years. In about 10% of patients, symptoms suddenly worsen.
It’s important to get diagnosed as early as possible with this disease, so don’t put off going to the doctor if you have any symptoms.
Diagnosis
The diagnosis of idiopathic pulmonary fibrosis is made only after other causes of symptoms have been ruled out. The first step in making a diagnosis of IPF is a complete history and physical exam. Your doctor also may order a variety of tests.
Breathing and Exercise Tests
Pulmonary function tests (or PFTs): These are breathing tests that are used to measure how much air the lungs can hold and well oxygen is moving into the bloodstream.
6-minute walk test: A six-minute walk test is used to see how far a patient can walk during six-minutes. A therapist keeps time while the patient walks as fast as possible. At many medical centers, heart rate and blood oxygen levels are recorded each minute of the test, but the main focus of the six-minute walk test is distance.
Oxygen titration test: During an oxygen titration test, the patient walks at their own pace while a therapist monitors blood oxygen levels. If the blood oxygen level drops below 89%, the patient is given supplemental oxygen, and the walk starts again. Walks keep going until the right amount of oxygen is given so the patient can walk for 6 minutes without blood oxygen dropping.
Imaging Tests
HRCT scan: Unlike a regular CAT scan of the chest, a high-resolution CAT scan (HRCT) is a special type of CAT scan that gives the clearest picture of ILD.
Many pictures are taken during an HRCT, some with the patient breathing in deeply and holding their breath, some with the patient blowing all their air out and holding their breath, and some with the patient lying face down.
Lab Tests
Arterial blood gas (or ABG): About ½ teaspoon of blood is taken from the wrist through a needle. Acid (pH), carbon dioxide, and oxygen levels are measured.
Blood tests: Blood from a vein is drawn through a needle and tested for things that may help explain the cause of the lung condition.
Procedures
Bronchoscopy with bronchoalveolar lavage: This test involves inserting a tube through the nose or mouth into the trachea (windpipe) so the doctor can see the airways, check for inflammatory cells in the lungs or sample small pieces of the lung to look for evidence of a specific ILD. In bronchoalveolar lavage a small amount of sterile saline or salt water is placed in one area of the lung and then withdrawn. The fluid contains cells that will be analyzed under a microscope. Small biopsy tools may be used through the bronchoscope if indicated.
GI tests: Sometimes patients will have tests to see if food or liquid is leaking into the windpipe (“down the wrong pipe”). This test may be called a tailored or modified barium swallow. A barium esophagram may be ordered to see if the esophagus (food tube) is moving swallowed food and liquid into the stomach like it should. Other tests may be ordered to measure pressure in the esophagus or to see if there is reflux (heartburn).
Surgical lung biopsy: This is an inpatient procedure done by a surgeon. Patients usually spend one or two nights in the hospital. During a surgical biopsy, the patient is given general anesthesia, and the thoracic surgeon removes pieces of lung tissue about the size of a quarter.
Treatment
The most appropriate course of treatment depends on the ILD diagnosis and its severity.
There is no formal staging system for IPF. But in general, IPF has the following stages:
- Recently diagnosed
- Needing oxygen with activity, but not at rest
- Requiring oxygen 24 hours a day: at rest, with activity, and during sleep
- Advanced oxygen needs
Different therapies may be recommended to try to slow worsening of the disease, to manage symptoms and to maintain quality of life.
Medications
As of January 2025, the U.S. Food and Drug Administration (FDA) has approved two medications for treatment of idiopathic pulmonary fibrosis (IPF) -- Nintedanib (Ofev®) and Pirfenidone (Esbriet®).
Nintedanib is oral medication that is taken twice daily. It blocks several pathways that lead to scarring. Nintedanib may cause diarrhea and, less commonly, nausea and vomiting.
Pirfenidone (Esbriet®) is an oral medication taken three times daily. It also blocks pathways that lead to scarring. Pirfenidone side effects include nausea, loss of appetite, upset stomach and photosensitivity (a tendency to easily sunburn, which can be severe).
Because of the potential side effects of these medications, your doctor will carefully monitor you while on drug therapy, which may include routine bloodwork.
In clinical trials, nintedanib and pirfenidone had equal effects of slowing disease progression.
Therapies
Pulmonary rehabilitation: Pulmonary rehabilitation (or pulmonary rehab) is a program for patients with any chronic lung condition, including IPF. Patients go to a pulmonary rehab center (which are sometimes linked to a hospital or larger medical center) 2 or 3 times per week for 6 to 12 weeks. The main part of pulmonary rehab is exercise, which is done with a therapist. Pulmonary rehab improves symptoms, physical functioning, strength, and quality of life. Pulmonary rehab is also offered virtually in some areas.
Oxygen therapy: Idiopathic pulmonary fibrosis can cause low levels of oxygen in the blood. Improving low levels of oxygen in the blood with supplemental oxygen can reduce strain on the heart and improve shortness of breath, fatigue and endurance. Some patients may need oxygen therapy all the time, while others may only need it during sleep or exercise. There are many different options for oxygen. A respiratory therapists will discuss what oxygen system will be the best fit for your lifestyle. Learn more about oxygen therapy. (link to supplemental oxygen section)
Lifestyle Management
No matter how severe idiopathic pulmonary fibrosis is, there are things that patients and their care team can do. Participating in the treatment plan will help people with IPF, their caregivers and family members achieve the best possible outcomes.
Things patients with IPF can do:
- Partner with your health care provider to create a comprehensive treatment plan.
- Learn more about IPF through trusted resources[SJ1] .
- Find ways to be more active. Dedicated exercise 5-6 days per week helps maintain muscle and heart fitness.
- Eat a healthy diet. There is no one diet that is best for patients with IPF. A good starting point is vegetables, nuts and seeds, lean meats, and minimal processed foods.
- Rest: Take a nap when needed.
- Maintain social interactions.
- Take steps to avoid infections: Get vaccinated. Wash hands frequently. Wear a mask when appropriate.
- If you smoke or vape, quit now. Call 1.800.QUIT.Now and/or ask your practitioner for help.
- Attend to your emotional/mental health.
- Take medication as prescribed.
- Use oxygen therapy as prescribed.
- Use breathing techniques to control breathing and speed recovery.
- Follow an action plan for the everyday and for exacerbations.
- Determine whether lung transplantation is an option for you. Talk to your practitioner, and use www.unos.org to learn more.
- Ask your practitioner about palliative care.Palliative care is simply care that focuses on keeping your quality of life as good as possible.
- Talk to your care/support team about the “what if’s”. As hard as it is for anyone to think about their death, it is important for you to decide what your goals are if your condition worsens. Let your care/support team know your goals.
Clinical Trials
Clinical trials help determine new treatment options for diseases and conditions. Patients with idiopathic pulmonary fibrosis have access to clinical trials and should speak with their physician to determine what trials might work best for them.
See a Specialist
If you or a loved one has idiopathic pulmonary fibrosis or a family history of IPF, it’s important to be evaluated and treated by an interstitial lung disease specialist.
National Jewish Health in Denver, Colorado, has one of the world’s largest interstitial lung disease treatment centers. Learn more about our Center for Interstitial Lung Disease or use the button below to schedule an appointment.
 Clinical Trials
Clinical Trials
For more than 100 years, National Jewish Health has been committed to finding new treatments and cures for diseases. Search our clinical trials.
