Signs You May Have an Immune Disorder
Published 4/7/26
 The immune system is your body’s natural defense against infection, but how do you know if it’s working the way it should? Some immune disorders make it harder to fight infections, while others cause the immune system to become overactive, attacking the body or triggering ongoing inflammation.
The immune system is your body’s natural defense against infection, but how do you know if it’s working the way it should? Some immune disorders make it harder to fight infections, while others cause the immune system to become overactive, attacking the body or triggering ongoing inflammation.
As allergist and immunologist Jessica Galant-Swafford, MD, explains, these conditions generally fall into two groups: immune deficiencies, which lead to frequent or severe infections, and immune dysregulation disorders, which can cause autoimmunity or unexplained inflammation.
Because symptoms can overlap with everyday illnesses, immune disorders are often missed or diagnosed late. Pay attention to patterns, such as
- How often you get sick
- How long symptoms last
- How your body responds to treatment
The following are key warning signs that may signal an underlying immune disorder and when it may be time to seek professional care.
You Get Sick More Often Than Expected
Everyone gets sick occasionally, especially during the winter season cold and flu season. But one of the most common signs of an immune disorder is getting infections more frequently than expected for your age and lifestyle.
According to Dr. Galant-Swafford, “Two or more pneumonias within a year in both children and adults warrants closer attention.”
It’s not just the number of infections that matters, but the overall pattern. Does it feel like you have a weak immune system? If illnesses seem to happen back-to-back, or you feel like you’re always recovering from something, your immune system may not be functioning effectively.
This is especially important if there’s no clear explanation for your illness, such as exposure to young children or a high-risk environment, such as working in a school or healthcare facility, frequenting airports, or taking other forms of public transportation
When infections become a regular part of life rather than an occasional inconvenience, it may be time to talk with a doctor about whether your immune system needs to be evaluated.
Infections Are Severe or Hard to Recover From
 Most common infections follow a predictable course: symptoms peak within a few days and gradually improve. But with immune disorders, recovery often doesn’t follow that pattern.
Most common infections follow a predictable course: symptoms peak within a few days and gradually improve. But with immune disorders, recovery often doesn’t follow that pattern.
“Patients with immune issues may be out of work for months, require repeated courses of antibiotics, or feel like they never fully recover,” said Dr. Galant-Swafford.
When these people are ill, instead of improving steadily, their symptoms may linger or worsen over time. A cold may turn into a prolonged illness, or a mild infection may escalate into something more serious.
This happens because a weak immune system struggles to clear the infection effectively, allowing inflammation and secondary infections to take hold.
If you find that routine illnesses consistently hit harder, last longer or require more aggressive treatment than expected, it’s an important signal that your immune system may not be responding normally.
You Develop Recurrent or Unusual Infections
Certain types of infections are red flags when they happen repeatedly or in unusual ways.
Dr. Galant-Swafford highlighted examples such as:
- recurrent pneumonia
- fungal infections,
- infections caused by organisms that typically don’t affect healthy individuals.
These are often referred to as “opportunistic” infections.
For example, fungal infections that spread beyond the mouth or skin, or infections like nontuberculous mycobacteria appearing in unexpected ways, may indicate a weak immune system.
Viral infections can reactivate or be more severe in individuals with immune disorders. For example, severe influenza requiring hospitalization or repeated episodes of shingles may suggest the immune system is not able to keep these viruses in check.
While a single unusual infection doesn’t necessarily mean there’s an immune disorder, a pattern of rare, severe or hard-to-treat infections should prompt further evaluation.
You Need Frequent or IV Antibiotics
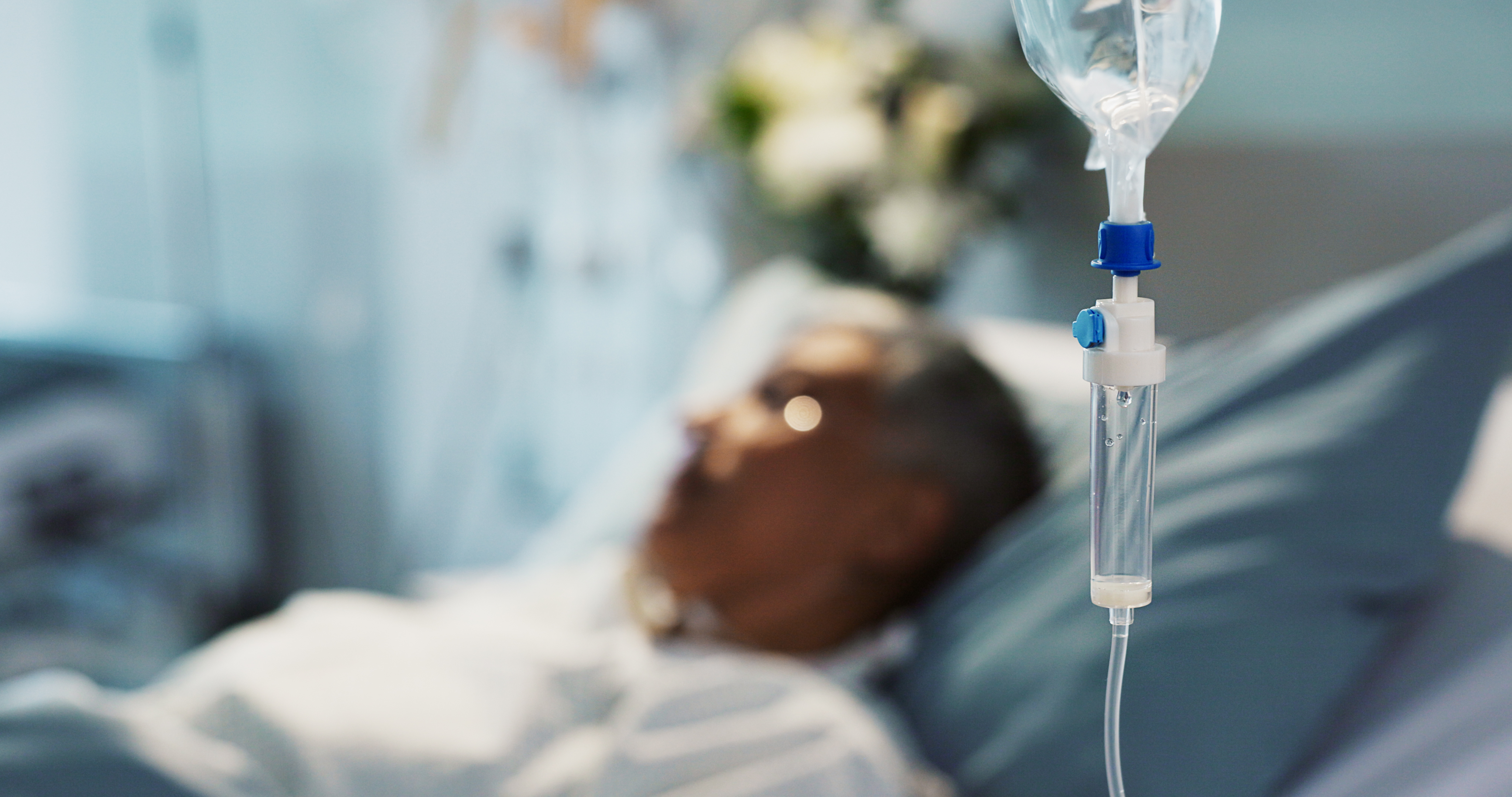 Most infections can be treated with standard, short courses of medication. But needing frequent antibiotics — or requiring intravenous (IV) antibiotics — is a major warning sign.
Most infections can be treated with standard, short courses of medication. But needing frequent antibiotics — or requiring intravenous (IV) antibiotics — is a major warning sign.
“A recurrent need for IV antibiotics is considered a significant red flag for immune deficiency,” said Dr. Galant-Swafford, as it suggests that infections are either unusually severe or not responding to typical treatment.
Repeated antibiotic use can also create a cycle: infections become harder to treat, and the body becomes more vulnerable to future illness.
If you find yourself needing multiple rounds of antibiotics for the same issue, or if infections escalate to the point of requiring hospital-based care, it’s important to look beyond the immediate illness.
These patterns often indicate that the underlying issue isn’t just the infection itself, but how the immune system is responding to it — by generating difficult-to-control inflammation throughout the body.
You Have Chronic Diarrhea or Unexplained Weight Loss
Digestive symptoms can also be a sign of immune dysfunction, especially when they are persistent or unexplained.
Chronic diarrhea that’s accompanied by weight loss is one of the classic warning signs of immune deficiency. In children, this may show up as failure to grow or gain weight. In adults, it may appear as ongoing gastrointestinal symptoms that don’t resolve.
These symptoms can result from infections the body cannot clear or from inflammation affecting the digestive system.
While many gastrointestinal conditions are common and not related to immune disorders, ongoing symptoms — especially when paired with infections or fatigue — should not be ignored.
If digestive issues are persistent, worsening or accompanied by weight loss, they may point to a deeper problem with immune function.
You Have Autoimmune Symptoms or Multiple Conditions
 In some immune disorders, the problem isn’t a weak immune system; it’s that the immune system is fighting the body itself.
In some immune disorders, the problem isn’t a weak immune system; it’s that the immune system is fighting the body itself.
“Autoimmune conditions occur when the immune system targets specific organs, such as endocrine organs (thyroid, pancreas), joints, gastrointestinal system (liver, colon) or the neurologic system,” said Dr. Galant-Swafford.
Having an autoimmune condition is relatively common. But developing multiple autoimmune diseases, especially at a young age, can be a warning sign of a broader immune disorder.
Symptoms vary depending on the condition but may include joint pain, fatigue, swelling or organ-specific issues. If autoimmune symptoms appear alongside infections or other unusual health patterns, it may point to a deeper issue with immune regulation.
Recognizing these connections can help ensure that underlying immune disorders are identified and treated appropriately. If you suspect you may have an autoimmune disease, you may benefit from scheduling an appointment with a rheumatologist, who will examine you and order the necessary laboratory testing to make a diagnosis.
You Experience Recurring Fevers Without a Clear Cause
Not all immune disorders involve infections. Some cause the immune system to become overactive, leading to repeated episodes of inflammation.
According to Dr. Galant-Swafford, these conditions can cause the body to act like it’s chronically infected, even when no infection is present.
A common sign is recurring fevers that come and go without a clear cause. These episodes may also include rashes, joint pain or abdominal discomfort.
Because tests may not show an infection, these symptoms are sometimes dismissed or misdiagnosed. But recurring, unexplained fevers that follow a recurring pattern can be an important clue to the possibility of what is called an “autoinflammatory syndrome.”
If you frequently feel like you’re getting sick but never receive a clear diagnosis, it may be worth asking whether inflammation, rather than infection, is the underlying issue.
Respond to Vaccines as Expected
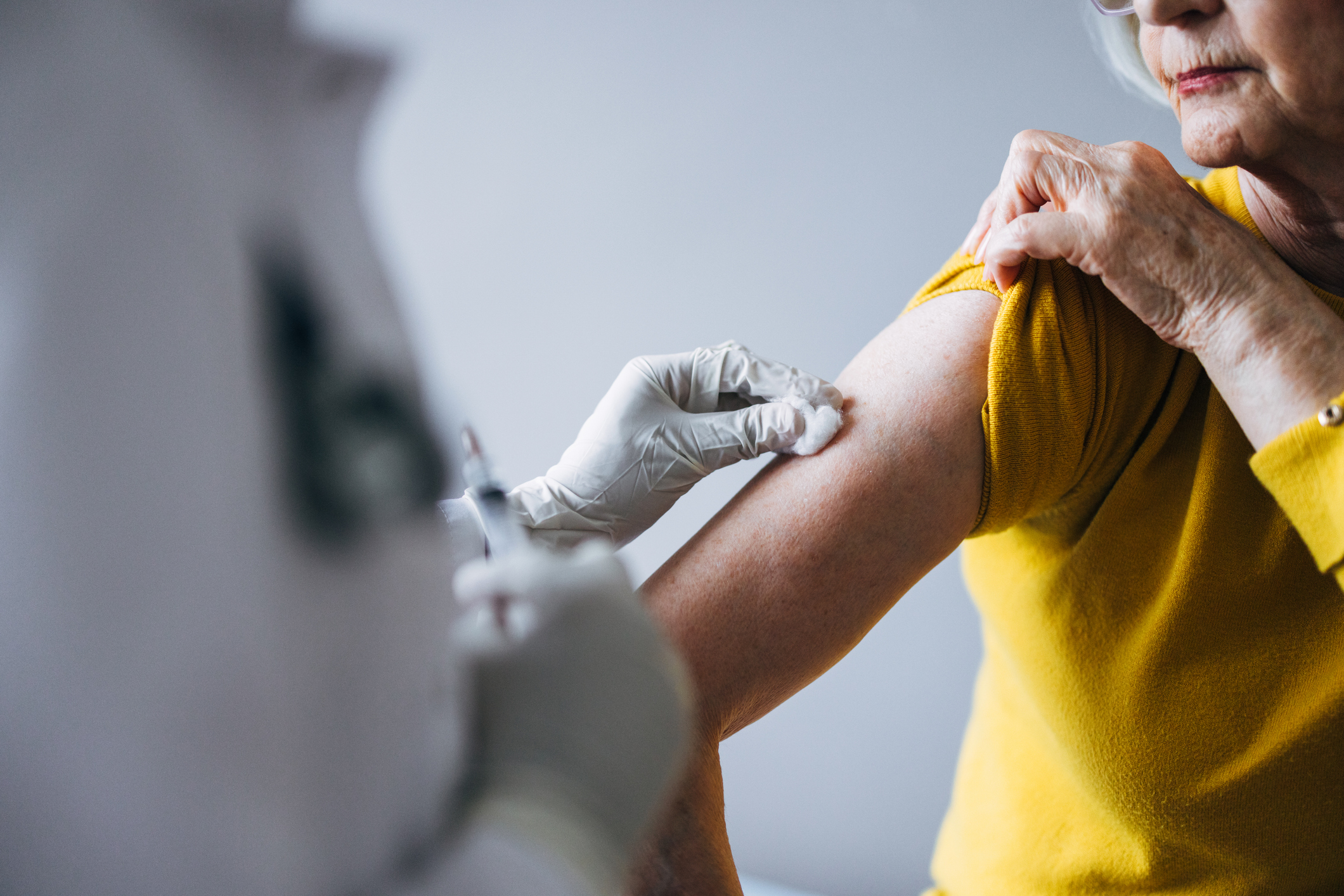 Vaccines are designed to train the immune system to recognize and fight infections. When they don’t work as expected, it can be a sign of an underlying problem.
Vaccines are designed to train the immune system to recognize and fight infections. When they don’t work as expected, it can be a sign of an underlying problem.
According to Dr. Galant-Swafford, “ineffective responses to immunizations specifically reduced immunity to that specific organism are a hallmark of immune deficiency disorders” For example, someone may receive multiple pneumococcal pneumonia vaccines but still develop a serious case of pneumonia from the bacteria S. pneumoniae.
This suggests the immune system isn’t producing a strong enough defense, even when properly stimulated. Laboratory studies can help to determine whether someone who has had a vaccine in the past mounted a protective immune response.
If you’ve had recommended vaccinations but still experience severe or repeated infections from those same diseases, it may be worth discussing immune testing with your doctor.
There’s a Family History of Immune Problems
Some immune disorders, particularly primary immune deficiencies, have a genetic component.
“A family history of immune deficiency can be an important indicator, especially when combined with symptoms like frequent infections or autoimmune conditions,” said Dr. Galant-Swafford.
If multiple family members have experienced unusual infections, immune disorders or unexplained inflammatory conditions, it’s crucial to share that information with your doctor.
Understanding family history can help guide testing, importantly genetic testing, and lead to earlier diagnosis, which can make a significant difference in managing immune-related conditions.
What to Do If You Think You Have an Immune Disorder
 If you recognize one or more of these signs, the next step is to document what’s happening and seek professional testing to understand how your immune system is functioning.
If you recognize one or more of these signs, the next step is to document what’s happening and seek professional testing to understand how your immune system is functioning.
You can start by speaking with your primary care provider, who may order initial labs or refer you to a specialist such as a clinical immunologist. Early evaluation can help identify treatable causes, prevent complications and provide a clearer plan for managing your health moving forward.
